Talking to Your Kids About Cancer
- Kay Wootten, a 57-year-old mom of three was diagnosed with stage 4 melanoma after a facial blemish doctors thought was eczema (an inflammatory skin condition that causes skin to become itchy and dry) turned out to be cancerous.
- Melanoma starts in the same cells that give your skin, hair, and eyes their color. Only, in melanoma, the cells change in a way that makes them able to spread to other organs. You're most likely to find melanoma on sun-exposed areas of skin, like your face, neck, arms, and legs.
- Parents living with cancer are encouraged to be as honest with their children as possible when explaining their condition with language that they can understand at their age.
- Here at SurvivorNet, we say that no one knows your body better than you, so if you feel like something is wrong, keep pushing.
Back in August 2018, Wootten first spotted the freckle-like mark on her face, however, it wasn’t until the 2020 Covid-19 lockdown that the blemish began to grow, itch, and bleed.
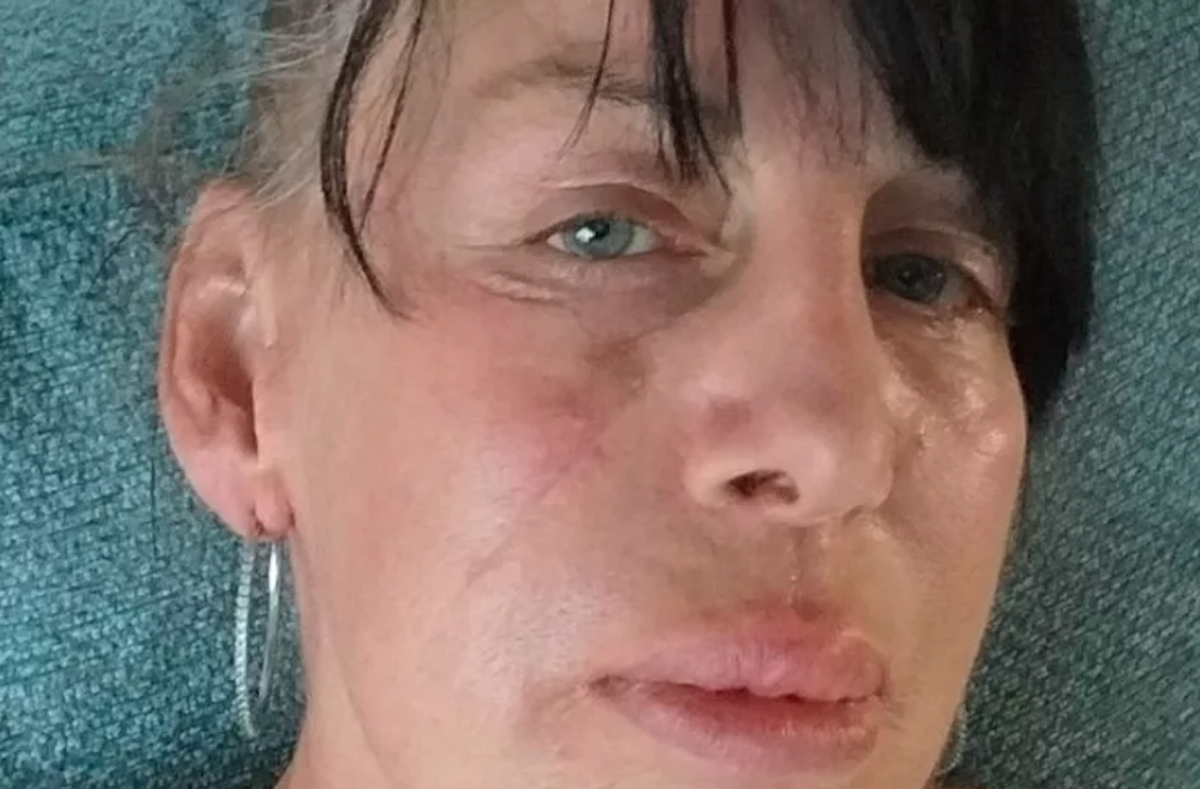
“All this could have been prevented if they just listened to me when it started to change,” Wootten told SWNS in a recent interview, according to the Daily Mail. “My whole life has completely changed. I try to joke it off but it’s really got me down.”
Expert Melanoma Resources
Wootten has since been going through chemotherapy treatments for the past year. She’s also had surgery to prevent further spread of the disease.
She told SWNS, “The first surgery I had was to remove the primary tumor and then they realized the margins around the tumor weren’t clear and still had cancer cells.
“I had more removed, and the margins still weren’t clear. I’ve had four cheek lifts in front of and under my ear and had a lymph node removed as well. I also had my thyroid removed as it was positive for melanoma.”
Wootten, noting how chemotherapy treatment has taken a toll on her body, added, “You don’t realize how much it affects your family as well. It’s not just you involved it’s your kids and you miss out on so much because of it.”
Understanding Melanoma
Melanoma starts in the same cells that give your skin, hair, and eyes their color. Only, in melanoma, the cells change in a way that makes them able to spread to other organs.
Changes to a mole you've had for a while or a new growth on your skin could be signs of melanoma, according to SurvivorNet's experts. Though it's unlikely that these marks are cancer, you'll want to keep an eye on them and let your doctor know about any changes you do notice.
WATCH: Dermatologist Dr. Cecilia Larocca On Why Getting Moles Evaluated Might Save Your Life
You're most likely to find melanoma on sun-exposed areas of skin, like your face, neck, arms, and legs. Surprisingly, you might also find them in places that have never been exposed to the sun, like:
- The palms of your hands or soles of your feet
- On your eyes or mouth
- Under your nails
Melanoma Treatment Options
Melanoma treatment has come a long way. Survival rates have risen dramatically, thanks to a “treatment revolution,” say SurvivorNet's experts. With breakthrough treatments like targeted therapy and immunotherapy now available, people who are diagnosed today have a much better chance of living a long and healthy life than ever before.
If you're diagnosed with melanoma, there's a good chance surgery is going to be the treatment your doctor recommends. In the early stages of the disease, removing the cancer should lead to a cure. The question is typically not whether you'll get surgery, but which kind you'll have.
WATCH: Dermatologic Surgeon Dr. Nima Gharavi, On The “Gold Standard Treatment” For Melanoma
For an early-stage melanoma that is close to the skin surface, Mohs surgery might be an option. This technique removes skin cancer, layer by layer, until all the cancer is gone.
In general, stage I melanoma surgery consists of the simple, in-office removal of the cancerous cells by a dermatologist. If the cancer is thicker, your surgeon will remove it through a technique called wide excision surgery.
The removal of stage II and III melanomas are performed by surgeons or surgical oncologists, not dermatologists. You may also have a sentinel lymph node biopsy to see if the melanoma has spread to the first lymph node where it's most likely to travel. If your cancer has reached this first lymph node, it may have spread to other neighboring lymph nodes, and possibly to other organs. Where the cancer is will dictate your treatment.
After surgery, the removed tissue and lymph nodes will go to a specialist called a pathologist, who will measure the melanoma and find out if it has clear margins. Having clear margins means the cells around the area of tissue that was removed don't contain any melanoma. When there aren't any cancer cells left around the removed area, your cancer is less likely to come back.
Top 5 Ways to Protect Your Skin
Once your cancer spreads, treatment gets a little more complicated, but there are still ways to stop it. New treatments have vastly improved the outlook for people with metastatic, or stage IV, melanoma.
Targeted drugs and immunotherapy have been shown to be more effective than chemotherapy. So, with many more choices, there is no standard treatment. Treatment will vary based on your condition and whether there is recurrent disease.
Research has found that immunotherapy drugs such as Keytruda (pembrolizumab) and Opdivo (nivolumab) helped some people live longer. Combining immunotherapy drugs Yervoy (ipilimumab) and Opdivo (nivolumab) has also extended survival. Opdivo (nivolumab) + relatlimab is a new therapy option added to the National Comprehensive Cancer Network guidelines in 2022. The combination of two immunotherapies is called Opdualag.
For those with the BRAF mutation, targeted drugs which shrink or slow the tumor can be a good option. This could include a combination of drugs, such as:
- Zelboraf (vemurafenib) and Cotellic (cobimetinib)
- Braftovi (encorafenib) and Mektovi (binimetinib)
- Tafinlar (dabrafenib) and Mekinist (trametinib)
- Zelboraf (vemurafenib) and Cotellic (cobimetinib) can also be combined with atezolizumab.
"Every patient is different and every situation is different," says Dr. Anna Pavlick, medical oncologist at Weill Cornell Medicine. She emphasized that "there is no cookie-cutter recipe," for treating stage IV melanoma.
There Is No "Cookie Cutter Recipe" for Treating Stage Four Melanoma
Dr. Pavlick also notes the importance of personalized care and treatment. "It really is a matter of looking at the tools we have so that we can pick the right tools to give the patient the best outcome.”
So, while there is no one-size-fits-all approach to treating metastatic melanoma, your doctor will work with you to develop a treatment plan that is tailored to your individual situation. Advances in research and technology are making the fight against metastatic melanoma more hopeful than ever.
The Importance of Advocating for Yourself
Although Kay Wootten was initially told her skin blemish was eczema, she knew something more was wrong with her body.
It's important to stand up for yourself, like Wootten did, if you feel that you're being dismissed or mistreated by a doctor. Getting a second opinion is crucial if something doesn't feel right. Luckily Wootten insisted on being referred to a dermatologist, and her cancer was ultimately caught, but it was stage four.
Here at SurvivorNet, we say that no one knows your body better than you, so if you feel like something is wrong, keep pushing.
Be Pushy, Be Your Own Advocate… Don't Settle
Dr. Zuri Murrell, a colorectal surgeon at Cedars-Sinai Medical Center, previously told SurvivorNet that sometimes, patients need to be pushy.
"From a doctor's perspective, every problem should have a diagnosis, a treatment, a plan for follow-up, and a plan for what happens next if the treatment doesn't work," Dr. Murrell said.
And as a patient, “if you don't feel like each of these four things has been accomplished, just ask! Even if it requires multiple visits or seeing additional providers for a second opinion, always be your own advocate.”
Tips for Parents Struggling to Talk About Their Cancer
After a cancer diagnosis, talking about it can be challenging, especially when children are on the other end of the conversation. It's important to prepare them for what might happen in the future, but you want to be gentle with this sensitive subject.
There is no single way to go about discussing cancer with children, as widower John Duberstein explains with SurvivorNet. Duberstein lost his wife to breast cancer, but before she passed away, the couple discussed her cancer with their children.
Talking to Kids About Cancer: Be Open as Much as You Can
“I think it's really important to be open with the kids as much as you can, as much as you feel like they can handle," Duberstein previously told SurvivorNet.
“When Nina started to look less like a cancer patient, the kids started to make unspoken assumptions about where Nina stood.”
He went on to say as parents, they had to counter false narratives, which developed in their children's heads about their mother's prognosis. They had to gently remind them her cancer was not going away.
“It was hard for them to hear even though they'd already been prepared,” he further explained.
If parents find themselves nervous before having this conversation, licensed clinical psychologist Dr. Marianna Strongin said children can pick up on your emotions, so it may help to check in with yourself beforehand.
"If at this moment, you are feeling scared, it might be helpful to calm and soothe yourself first before speaking to your child," she said.
"Having these conversations may bring up deep emotions you may have stowed away. There is nothing wrong with showing our emotions to children as long as we can remain calm and give them a sense of safety," she said.
Helping them feel safe can mean giving them tools and strategies to manage their feelings about the situation.
"I love using my childhood self when explaining anything to children," Strongin said. "I might say, 'when I was your age, I remember feeling scared of many things, but one thing that always helped is taking three very deep breaths and telling my body it will be okay.'
"It is these kinds of dialogues that allow our children to feel safe and in control."
Contributing: SurvivorNet Staff
Learn more about SurvivorNet's rigorous medical review process.

