Understanding Acral Lentiginous Melanoma (ALM)
- Laura Jennings was diagnosed with a rare type of melanoma at 40 years old, after doctors dismissed a strange “bruise”-like mark on her toenail as a fungal infection.
- She ultimately had the cancer removed, later learning it didn’t spread. But now she’s urging others to push for answers and get checked when something seems off with your body.
- Jennings was diagnosed with acral melanoma, which is sometimes called acral lentiginous melanoma (ALM). As per research published in the medical journal Neoplasia, acral melanoma “arises on the non-hair bearing skin of the nail bed, palms of the hand and soles of the feet” and is not linked to sun ultraviolet (UV) light like other skin cancers.
- This rare type of skin cancer is more commonly found in people of color and older adults. It’s the type of cancer which led to Bob Marley’s death. However, the type of cancer can happen to anyone. So it’s important to be aware of the signs.
- Melanoma starts in the same cells that give your skin, hair, and eyes their color. In melanoma, the cells change in a way that allows them to spread to other organs. The most important thing to look out for when it comes to finding melanoma early is a new spot on your skin or a spot changing in size, shape, or color.
Recalling how she’s often “clumsy” and “fairly active,” she wrongly presumed the mark on her toe was a bruise — prompting her to simply cover it with nail polish.
Read More
However, since getting an in-person doctor’s appointment was difficult for her in the wake of the Covid-19 pandemic, she was able to make a virtual appointment with her doctor and was misdiagnosed with a fungal nail infection.
It wasn’t until the spring of 2023 that her symptoms worsened.
After noting how “no one ever tells you to look out for this,” referring to her toenail symptoms, she then “pushed for a face-to-face appointment.”
She explained further, how the next doctor she saw “knew straight away that this could be something much more serious” and referred her to a dermatologist.
Jennings then had the tumor on her toenail removed and has much of the surrounding area needed. A biopsy then revealed she had Acral Lentiginous Melanoma.
According to the AIM At Melanoma foundation, Acral lentiginous melanoma (ALM) is a form of melanoma that typically develops on the palms, soles, or beneath the nails. The term “acral” is derived from Greek and relates to the extremities—specifically the hands and feet—where this melanoma most often occurs. “Lentiginous” describes the characteristic dark pigmentation of the affected area, which is usually noticeably darker than the surrounding skin.
The foundation explains, “Acral lentiginous melanoma (ALM) can be difficult to diagnose” and most often develops on or around hands and feet, or in nail beds. Like superficial spreading melanoma, ALM grows on the surface of the skin or under the nail bed before becoming invasive.
“ALM sometimes develops from an existing mole. It can also occur seemingly out of nowhere on healthy skin.”
In Jennings’ case, she needed a portion of her toe amputated to remove the cancer and a lymph node in her groin surgically removed to check if the cancer had spread elsewhere.
She ultimately had the cancer removed and her doctors informed her that the cancer didn’t spread to her lymph nodes.
However, she will have followup appointments over the next three years until she can be confirmed to be “clear” of the disease.
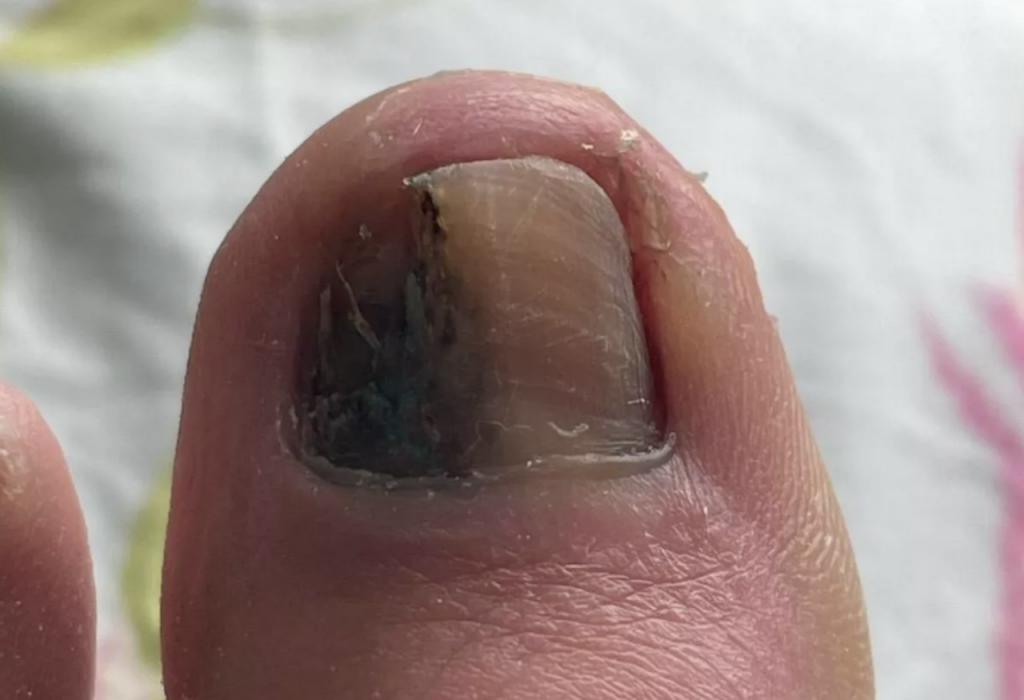
In an effort to spread awareness on this specific type of melanoma, Jennings said, “Friends will ask what I think if they have a mark on a nail, and I say, ‘I’m not a doctor, but what I think is you should go and get it checked if you’re worried.’
“Because if something is not normal about your nails, you must get it checked. It might be a fungal nail infection, it might be because you banged it with something. But it could be something more. Early detection really is key.”
As for how Jennings’ recovery went, she said “My fantastic consultant is also a plastic surgeon, so it doesn’t look bad at all. In fact, lots of people don’t really notice.
“It’s like I’ve just got a shorter toe and no toenail.”
She concluded, “Every single day is very important to me, and actually, I think having a visible reminder of what I’ve been through is important.
“It’s a daily reminder of how precious life is, that encourages me to make the most of every day, every opportunity to celebrate and most of all, life’s simplest pleasures. Because after all, life isn’t a dress rehearsal.”
Understanding Acral Melanoma
According to the Melanoma Research Alliance, acral melanoma, which is sometimes called acral lentiginous melanoma, is “a rare subtype of melanoma that forms on the palms, soles of feet, or under finger or toe nails.
This form of cancer, which led to iconic reggae singer Bob Marley’s passing, differs from skin melanoma, as it’s not believe to be cause by sun exposure and is often found in areas not normally exposed to UV rays.
Am I at High Risk for Melanoma?
According to research published in the medical journal Neoplasia, acral melanoma “arises on the non-hair bearing skin of the nail bed, palms of the hand and soles of the feet” and is not linked to sun ultraviolet (UV) light like other skin cancers.
This rare subtype of melanoma is more common among people of Black, Hispanic/Latin, and Asian descent, and older adults.
Expert Melanoma Resources
- Atypical Moles Don’t Necessarily Mean You Have Melanoma
- Beating Aggressive Melanoma: An Immunotherapy Success Story
- Dramatic Improvement in Melanoma Survival Rates– The Treatment Revolution is Working
- Examining Your Skin for Melanoma: Remember ABCDE
- Melanoma Relapse Treatment: Advances on the Horizon
- More Men Are Dying From Melanoma Across Globe, While More Women are Surviving
- Skin Cancer Awareness Month: Be On the Lookout for These Not-So-Common Signs of Melanoma
“Acral melanoma is a rare form of melanoma, accounting for only about 1-3% of all cases diagnosed. About 2,000 – 3000 cases of acral melanoma are diagnosed each year in the United States,” the Melanoma Research Alliance explains.
RELATED: Myth Busting: My Fingernails Have Streaks … Do I Have Cancer?
The alliance points out that symptoms can vary, but can include:
- A gray, tan, black or brown spot; or discoloration on the palms of the hands or soles of the feet.
- Any changing spot growing on hands or feet.
- A new or changing mole on the hands or feet.
- Discolorations or dark streaks found vertically across toenail or fingernail beds.
- A spot or patch on the hands or feet that itches, bleeds, or is painful
WATCH: How do you perform a skin check using the ABCDEs?
What to Look for When Checking Your Nails for Cancer
When it comes to examining yourself for skin cancer, it’s natural (and obvious) to check your skin and moles. But check your finger and toenails for signs of skin cancer, too.
When checking your nails for melanoma skin cancer, look for the following indicators:
- Dark streak: This could look like a brown or black band in the nail, according to the American Academy of Dermatology, oftentimes on the thumb or big toe of your dominant hand or foot. But a dark streak can show up on any nail.
- Dark skin next to your nail: When the skin around your nail becomes darker, it could be a sign of advanced melanoma.
- Nail lifting from your fingers or toes: When this happens, your nail starts to separate from the nail bed; the white free edge at the top of your nail will start to look longer as the nail lifts.
- Nail splitting
- Nodule or bump under your nails: It’s possible that you could also see a band of color on your nail; it could be wide and irregular, or dark and narrow.
RELATED: Get Your Moles Evaluated to Rule Out Melanoma
Dr. Dendy Engelman, a board-certified dermatologic surgeon and associate at Manhattan Dermatology and Cosmetic Surgery, previously told SurvivorNet it’s also possible that getting your nails done at the salon could increase skin cancer risk.
“The reality is, if we have our hands or feet under these ultraviolet lamps without protection, we’re exposing the dorsum of the hands or foot, the skin around the nails, to this UV light,” she said. “That, over time, can increase our risk of skin cancer.”
RELATED: Myth Busting: My Fingernails Have Streaks … Do I Have Cancer?
The Melanoma Workup
It’s important to understand there are regular skin checks for cancer at the dermatologist and also thorough melanoma checks—which are very different.
Unlike other diseases, the workup for melanoma is pretty straightforward. For any skin lesions, your dermatologist will give you a head-to-toe visual examination to look for any other atypical moles or suspicious lesions.
If a growth warrants further evaluation, you might get a biopsy. And if advanced melanoma is found, you may need additional imaging and blood tests to help determine the best treatment plan.
Blood tests may include:
- Complete blood count (CBC): looks at the number and types of cells in your blood, including red blood cells, white blood cells, and platelets
- Comprehensive Metabolic Panel (CMP): measures the blood levels of certain enzymes, proteins, electrolytes, and minerals
- Lactate dehydrogenase (LDH): an enzyme that’s increased in many cancers
Imaging tests may include:
- CT scan: uses x-rays and a computer to create detailed images of your body
- PET scan: uses radioactive materials (called tracers) and a special camera to create pictures of areas inside the body where cancer may be growing
- MRI: Uses radio waves and magnets to create images of organs and tissues
A pathologist may also examine your tissue sample under a microscope to look for certain mutations. This is called biomarker testing, which helps determine the best treatment options for you. The BRAF mutation is the most common mutation found in melanoma tumors.
It’s important to remember that many atypical skin lesions are not cancer. So don’t worry if your doctor finds something that looks a bit strangeit may just be a benign growth. If you have any concerns about the findings, be sure to talk with your doctor.
Turning to Immunotherapy to Treat Melanoma
Immunotherapy helps patients fight melanoma by enabling their own antibodies to attack cancer cells, and it’s important to understand that immunotherapy several medications are available to patients. Some people may not be candidates for this therapy, and side effects vary from person to person.
“When immunotherapy came on the market, it was such an exciting time for everyone involved in the care of melanoma, the main reason being is it went from this scary unmanageable cancer with no treatments to one that could potentially have a long-lasting result with patients absolutely never having to worry about their melanoma,” explains Dr. Cecilia Larocca, a dermatologist at Dana Farber Cancer Institute.
FDA-Approved Immunotherapy for Melanoma
There are several FDA-approved immunotherapies for melanoma. Each is approved for certain instances of melanoma.
- Tebentafusp-tebn (Kimmtrak)
- Aldesleukin (Proleukin)
- Atezolizumab (Tecentriq)
- Dostarlimab (Jemperli)
- Interferon alfa-2b (Intron A)
- Ipilimumab (Yervoy)
- Nivolumab (Opdivo)
- Peginterferon alfa-2b (Sylatron/PEG-Intron)
- Pembrolizumab (Keytruda)
- Talimogene laherparepvec (Imlygic)
- Imiquimod (Aldara)
WATCH: Turning to Immunotherapy.
Questions to Ask Your Doctor
If you are diagnosed with skin cancer, you may have some questions for your doctor. SurvivorNet suggests some of the following to help you on your cancer journey.
- What type of skin cancer do I have?
- What treatment options exist for my type of melanoma?
- Will this treatment be covered by insurance?
- Would treatment through a clinical trial make sense to me?
- What resources exist to help manage my anxiety because of this diagnosis?
Contributing: SurvivorNet Staff
Learn more about SurvivorNet's rigorous medical review process.

