Navigating an Aggressive Skin Cancer Diagnosis
- “Real Housewives of Beverly Hills” alum Teddi Mellencamp, 44, continues to navigate stage 4 melanoma, an aggressive form of skin cancer, including the spread of 10 non-cancerous but disruptive brain lesions, according to her Rock and Roll Hall of Fame father, John Mellencamp, 74. Teddi says scans from November showed “no detectable cancer” at the moment, but she continues treatment.
- She has been open about the physical and emotional toll of immunotherapy (which uses reengineering immune cells from the patient to fight the cancer). Its side effects include fatigue, nausea, joint pain, and changes in blood counts.
- Clinical trial results from last year show that using the immunotherapy drug pembrolizumab (Keytruda) before and after surgery can reduce the risk of melanoma recurrence by 42%, a potential shift toward a new standard of care for high-risk patients.
- “It’s important that patients and physicians are aware of this study as it represents a new potential standard of care,” says Dr. Janice Mehnert, associate director of clinical research at NYU Langone’s Perlmutter Cancer Center.
- Experts like Dr. Nima Gharavi, Director of Dermatologic Surgery at Cedars-Sinai, note that while immunotherapy has transformed melanoma treatment, surgery—often with wide margins or Mohs surgery for early, surface-level cases—remains the cornerstone of care.
“She has 10 lesions in her brain … even though the lesions are not cancerous right now, they still interrupt her thinking, and it’s in her frontal lobe,” John Mellencamp told People Magazine.


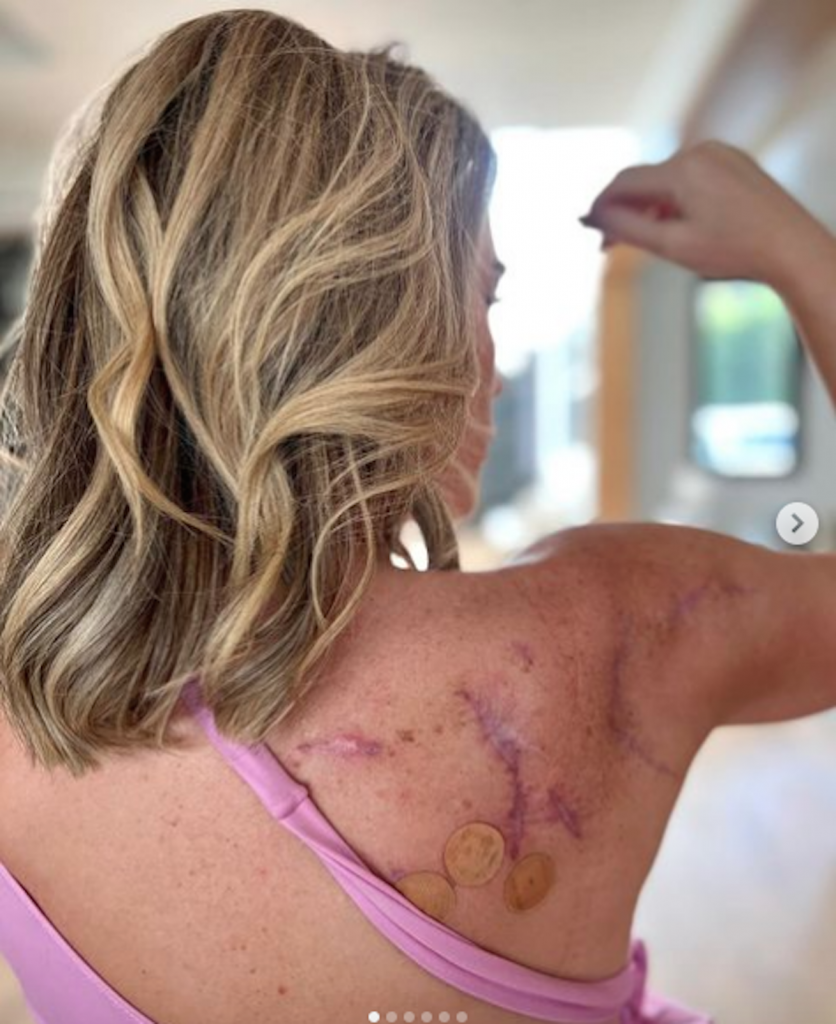
“Some days are definitely better than others,” she said.
“You don’t see all the times I’m lying in my bed, unable to do much. Don’t be afraid to let people know how you’re feeling, and don’t feel guilty if you need to rest.”
A clinical trial studying the impact of high-risk melanoma patients using the immunotherapy agent pembrolizumab (brand name: Keytruda), used before and after surgery, reduces the risk of tumor recurrence.
The group treated in the trial before and after surgery saw a 42% lower rate of cancer‑related “events,” such as the cancer returning.
“It’s important that patients and physicians are aware of this study as it represents a new potential standard of care,” says Dr. Janice Mehnert, associate director of clinical research at NYU Langone’s Perlmutter Cancer Center.
“For patients with high-risk disease, delivering immunotherapy prior to surgery must be considered.”
Dermatologist Dr. Cecilia Larocca of Dana-Farber Cancer Institute told SurvivorNet that immunotherapy transformed melanoma care.
WATCH: The Side Effects of Immunotherapy.
“When immunotherapy came on the market, it was such an exciting time for everyone involved in the care of melanoma… it went from this scary, unmanageable cancer with no treatments to one that could potentially have a long-lasting result,” explained Dr. Cecilia Larocca, dermatologist at Dana-Farber Cancer Institute, in an interview with SurvivorNet.
Still, side effects are common and can include fatigue, nausea, joint pain, and changes in blood counts. In rare cases, patients may experience severe reactions that require stopping treatment.
Although other forms of treatment, including immunotherapy, are treatment options depending on the patient’s specific diagnosis, Dr. Nima Gharavi, Director of Dermatologic Surgery at Cedars-Sinai, says, “The gold standard for treatment of melanoma is surgical treatment with wide margins.”
In some cases of early-stage melanoma that’s close to the skin’s surface, Mohs surgery may be offered. This is most common in areas such as the face, ears, and nose.
Expert Resources on Melanoma Treatment
- ‘A Game Changer’: New Combination Immunotherapy for Advanced Melanoma Offers More Options For Patients
- A Biopsy of Your Mole Doesn’t Mean You Have Melanoma
- A Melanoma Vaccine for Metastatic Patients
- Am I at High Risk for Melanoma?
- An Immunotherapy Success Story: Mary Elizabeth Williams Lived Through Metastatic Melanoma
- Criteria and Considerations for Using Newly FDA-Approved Lifileucel in Advanced Melanoma
- How is Melanoma Treated After Surgery? The Landscape of Therapies Explained
Mohs Micrographic Surgery: A Precise Approach to Skin Cancer Treatment
Mohs surgery is the leading method for treating skin cancer on delicate, high-risk areas like the face, ears, and nose. This meticulous technique—known as Mohs micrographic surgery (MMS)—uses microscopic guidance to remove cancerous tissue layer by layer, ensuring that only affected areas are excised while preserving as much healthy skin as possible.
WATCH: The best surgery option for melanoma.
During the procedure, the area is numbed with a local anesthetic. The surgeon carefully removes the visible tumor with a scalpel and immediately examines the tissue under a microscope. If cancer cells remain, the process is repeated—one layer at a time—until all cancerous cells are gone.
This methodical approach offers high cure rates, particularly when cancers are caught early, and minimizes scarring for sensitive, visible areas of the body.
“What is being done is that you’re able to remove a very conservative margin around the cancer and study it in, essentially, real time,” explains Dr. Sumaira Aasi, a professor of dermatology and Director of Mohs and Dermatologic Surgery at Stanford.
View this post on Instagram
“The Mohs surgeon will take a conservative cut circumferentially around the cancer, where we’re able to preserve healthy tissue. We’re able to process the tissue and look at the cancerous tissue and know where there are still tumor cells persisting. As the Mohs surgeon removes the cancer, it’s mapped out.”
Dr. Aasi adds that the surgeon may go back specifically to the areas where the cancer cells were present and take out another conservative margin or amount of cancerous tissue, and repeat the process until the cancer is out completely.
Immunotherapy Side Effects During Treatment for Melanoma
A new study published in JAMA Oncology is shedding light on the long-term side effects of immunotherapy in melanoma patients—revealing that chronic complications may be more widespread than previously thought.
“Chronic and long-lasting side effects were more common than we expected and involved a variety of often overlooked organs like the thyroid, salivary glands, and joints,” said Dr. Douglas Johnson, senior author of the study and associate professor of medicine at Vanderbilt University Medical Center.
WATCH: Tell Your Doctor About Immunotherapy Side Effects
Despite the findings, Dr. Johnson emphasized the groundbreaking nature of immunotherapy, especially anti-PD-1 drugs. “It has been an absolute game-changer for patients with melanoma,” he noted. “I think the first thing to recognize is how really transformative the Anti-PD-1 drugs have been… patients can have very long-term responses to treatment.”
Still, for patients with advanced melanoma—especially those who’ve undergone surgical removal and have a low risk of recurrence—Dr. Johnson advised more nuanced conversations around treatment. “So determining whether the risks of the side effects, weighing the benefits of treatment with the risks of the side effects, can be an important consideration,” he said. “What our study did was we basically saw that some of these side effects were more common, really, than had been previously reported.”
Reported side effects can range from mild to severe, including dry throat, inflammation of the eye blood vessels, numbness, or tingling. And for many, the decision comes down to weighing symptom severity with potential longevity benefits.
WATCH: Managing Immunotherapy side effects.
Dr. Anna Pavlick, another expert in melanoma care, added context around immunotherapy management. “Depending upon the severity, it depends upon how we manage it,” she said.
“The percentage of patients who have very serious side effects from immunotherapy is contingent upon whether patients will get one medicine or a combination of two medicines.”
She explained that patients receiving a single immunotherapy drug face a 10–15% chance of experiencing severe reactions like rash or diarrhea. But for patients with metastatic melanoma, a dual-drug regimen—though more effective at controlling the cancer—comes with about a 50% chance of developing side effects.
FDA-Approved Immunotherapy for Melanoma
There are several FDA-approved immunotherapies for melanoma. Each is approved for certain instances of melanoma.
- Tebentafusp-tebn (Kimmtrak)
- Aldesleukin (Proleukin)
- Atezolizumab (Tecentriq)
- Dostarlimab (Jemperli)
- Interferon alfa-2b (Intron A)
- Ipilimumab (Yervoy)
- Nivolumab (Opdivo)
- Peginterferon alfa-2b (Sylatron/PEG-Intron)
- Pembrolizumab (Keytruda)
- Talimogene laherparepvec (Imlygic)
- Imiquimod (Aldara)
The goal is to steadily reduce the risk of recurrence in all patients. It’s not a one-size-fits-all approach. Some people may not be candidates for this therapy, and side effects vary from person to person.
Understanding Melanomas
Melanoma starts in the same cells that give your skin, hair, and eyes their color. In melanoma, the cells change in a way that allows them to spread to other organs.
Changes to a mole you’ve had for a while or a new growth on your skin could be signs of melanoma, according to SurvivorNet’s experts. You’ll want to watch them and tell your doctor about any changes you notice.
WATCH: How do you perform a skin check using the ABCDEs?
SurvivorNet experts recommend avoiding unprotected sun exposure because ultraviolet (UV) radiation can lead to melanoma. Tanning beds pose ultraviolet radiation risks for skin cancer and should be avoided. Many dermatologists recommend using spray tans to reduce the risk of melanoma skin cancer.
The most important thing to look out for when it comes to finding melanoma is a new spot on your skin or a spot that is changing in size, shape, or color, SurvivorNet’s medical experts say.
Treatment options for melanoma include targeted therapy and immunotherapy, which give people a better chance of living a long and healthy life than ever before. If you’re diagnosed with melanoma, there’s a good chance surgery will be the treatment your doctor recommends.
Cancer removal usually leads to a cure in the early stages of the disease. After surgery, the removed tissue and lymph nodes are examined to measure the melanoma and determine if it has clear margins. Clear margins mean the cells around the area of tissue that was removed don’t contain any melanoma. When no cancer cells are left around the removed area, your cancer is less likely to return.
WATCH: Beating Aggressive Melanoma: An Immunotherapy Success Story
For melanoma patients who need additional treatment after surgery, they are likely to receive adjuvant therapy (treatments administered after surgery). Adjuvant therapy is designed to improve outcomes and decrease the risk of recurrence.
Questions to Ask Your Doctor
If you are diagnosed with skin cancer, you may have some questions for your doctor. SurvivorNet suggests the following to help you on your cancer journey.
- What type of skin cancer do I have?
- What treatment options exist for my type of melanoma?
- Will insurance cover this treatment?
- Would treatment through a clinical trial make sense for me?
- What resources exist to help manage my anxiety because of this diagnosis?
Contributing: SurvivorNet Staff
Learn more about SurvivorNet's rigorous medical review process.

