Nicole Eggert Embraces Advocacy After Second Mastectomy, Inspiring Preventive Living
- Nicole Eggert, 53, recently underwent her second mastectomy (removal of the breast) and has embraced advocacy, becoming a SurvivorNet Breast Cancer Awareness Ambassador and sharing her journey at the San Antonio Breast Cancer Symposium.
- SurvivorNet’s Breast Cancer Dialogues provides a community where survivors’ stories shine, helping women feel supported as they face treatment choices, manage side effects, and adjust to life after care.
- Eggert says she’s taking a few cancer medications as part of her treatment. One of them is Ribociclib (Kisqali), a targeted drug that targets specific proteins known as the cyclin-dependent kinases 4 and 6, abbreviated as CDK4/6, which are crucial in cancer cell division and growth.
- Dr. Eleonora Teplinsky, Head of Breast Medical Oncology at Valley Health System, explains that during phase III clinical trials, patients who received Ribociclib and endocrine (hormone) therapy at three years, their disease-free survival was 90.4% compared to 87.1% in the group that received endocrine therapy alone.”
- Eggert says her treatment is causing some lingering side effects, including aches, hair loss, and dry skin. However, she remains optimistic, viewing them as manageable sacrifices if it means keeping cancer away.
- Despite the challenges of treatment, Eggert stays hopeful about the future, drawing strength from her desire to be present for her children and crediting SurvivorNet as a vital “lifeline” throughout her cancer journey.
Since being diagnosed in late 2023, Eggert has embraced her role as a fighter, finding strength in vulnerability and purpose in advocacy. “I want to have all of the hard conversations, but make those hard conversations less hard. I just want to show up and do my part,” she told SurvivorNet.
Read More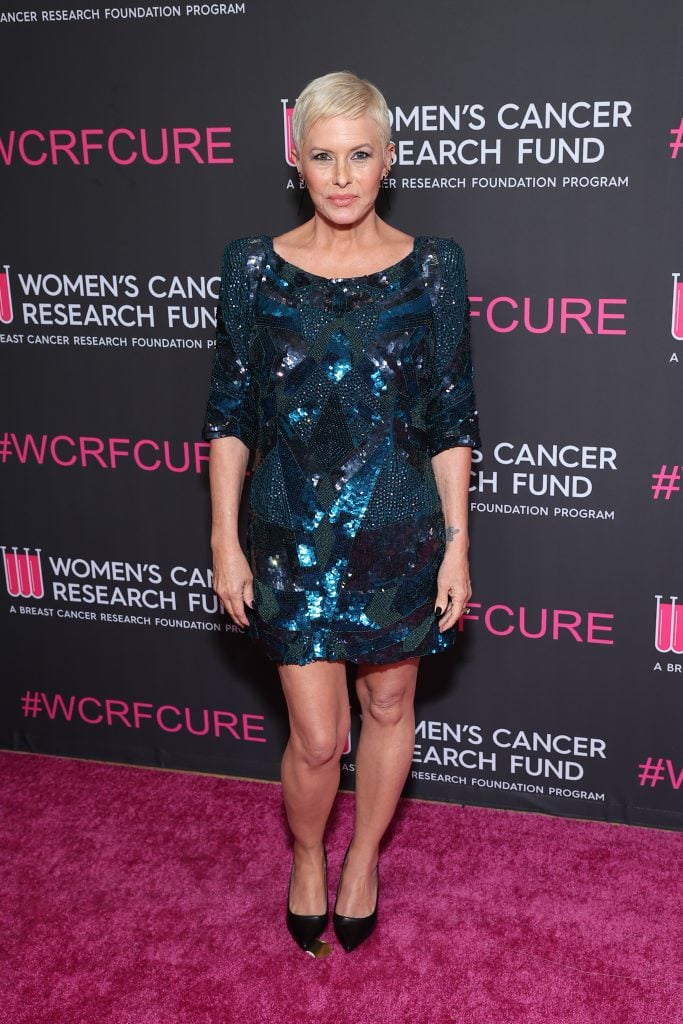
Eggert hopes her openness inspires a shift in perspective: “I want to push forward that this can be life-changing in the best possible way. I have my weak moments, I have my breakdowns, and I live in a little bit of fear—it could come back. But you begin to live in this space of ‘what if’ and embrace a preventative lifestyle. I want to encourage everyone, with or without cancer, to live that way.”
In early autumn, Eggert had her second mastectomy followed by breast reconstruction.
Dr. Sarah Cate is Chief of Breast Surgery at Stamford Hospital. She says a mastectomy procedure has very specific indications.
“Some of the things that would call for a mastectomy are things like a large tumor size to breast ratio, or having cancer in more than one area of the breast, or things like a genetic mutation,” Dr. Cate explained to SurvivorNet.
The reconstruction process can happen at the time of the surgery to remove the breast, or later on in the case of implants.
WATCH: Breaking Down Breast Reconstruction Options
When it comes to breast reconstruction, “there are really two main ways to do it,” says Dr. Andrea Pusic, Chief of Plastic and Reconstructive Surgery at Brigham and Women’s Hospital in Boston.
“One is using a woman’s own tissue, and the other is using breast implants. So, starting with the use of your own tissue option. Most commonly, we use the tissue from the lower tummy area. It’s called the TRAM flap, or you’ll hear DIEP flaps or pedicle TRAM flaps,” Dr. Pusic explained.
“What that means is, we’re taking the same kind of tissue that will be in a tummy tuck– so everything sort of below the belly button– that tissue is removed and brought up to make the breast,” Dr. Pusic continued.
WATCH: Breast Reconstruction: Regaining Your Sense of Self
Dr. Pusic says breast reconstruction using implants is a two-step process.
“The first step involves placing a tissue expander, which can be done at the same time as the mastectomy. The expander is positioned either beneath the pectoralis muscle or, increasingly, above it. Over time, the expander gradually stretches the remaining skin. Then, months later, the patient typically returns to have the expander replaced with a permanent implant.”
As for Eggert, she admits she’s pleased with how her breasts look after the procedure, but she can feel the difference.
“Aesthetically, I look amazing [after my second mastectomy]. However, they don’t feel as great as they look. I have one Barbie boob, and I have a natural boob that’s been made to look like the Barbie boob, and both are numb,” Eggert explained to SurvivorNet.
Expert Resources for Early-Stage Breast Cancer
- Introduction to Early-Stage Breast Cancer
- NATALEE Trial Supports Use of Kisqali with HR+/HER2- Early-Stage Breast Cancer at Increased Risk of Recurrence
- More Than 80% of Women With Early-Stage Triple-Negative Breast Cancer Experienced a Prolonged Event-Free Survival With Keytruda Plus Chemotherapy Regimen
- Early Stage Breast Cancer: What to Know About Testing
- ‘A Real Milestone’: FDA Approves New After Surgery Treatment for High-Risk Early Breast Cancer
Eggert’s Ongoing Breast Cancer Treatment
When Eggert bravely went public with her diagnosis, she revealed she had stage 2 cribriform carcinoma breast cancer. Early-stage breast cancer refers to cancer that is typically smaller in size and confined to the breast and surrounding tissue.
The “Baywatch” alum says she’s currently taking a few cancer medications, including Kisqali, Letrozole, and Zoladex.
WATCH: How The Drug Kisqali and Endocrine Therapy Work For Hard-To-Treat Breast Cancers
What is Kisqali?
Ribociclib (Kisqali) belongs to a class of medications known as kinase inhibitors, which block the actions of kinases, a type of protein in cells that play a key role in growth, metabolism, and cell repair. Inhibiting the kinase in cancer cells slows down the cancer from growing and spreading.
Kisqali is usually taken once daily in pill form along with the non-steroidal aromatase inhibitor (NSAI) hormone therapy.
Doctors determine what type of cancer a patient has before treatment with a test called a biopsy. This involves removing a small sample of the tumor for testing in the lab.
If a patient’s disease is metastatic, hormone receptor positive, HER2 negative, then the combination therapy can even be considered as a first-line treatment, meaning it is the first treatment doctors will use.
Analyzing data from the NATALEE phase III clinical trial, Dr. Eleonora Teplinsky, Head of Breast Medical Oncology at Valley Health System, explained how breast cancer patients who received Ribociclib along with endocrine therapy (the current recommended treatment) had a 25% lower risk of recurrence or death.
Prior to the study, “Ribociclib was already approved for metastatic hormone receptor-positive breast cancer, but this study was looking to see if it has benefits in reducing recurrence in earlier-stage breast cancer,” Dr. Teplinsky explained.
The study looked at something called disease-free survival, which means patients are alive without their cancer recurring.
“In the group that received Ribociclib and endocrine therapy … at three years their disease-free survival was 90.4% compared to 87.1% in the group that received endocrine therapy alone,” Dr. Teplinsky said. This translates to a 3.3% “absolute improvement.”
WATCH: NATALEE Trial for Breast Cancer
How Does Kisqali Work?
Cancer cells divide and grow by repeatedly going through a series of proliferation events called the “cell cycle.” This cycle is highly complex and regulated, meaning that several proteins within the tumor cells must be activated in a specific way at specific times for the cells to proliferate. CDKs, including CDK4/6, are just such proteins. They control key events in the cell cycle pathway, which makes them great targets for anti-cancer drugs, such as CDK inhibitors, which is the class of drugs Kisqali belongs to.
WATCH: What Are CD4/CD6 Inhibitors? And How Can They Fight Advanced Breast Cancer?
Kisqali, however, cannot work alone. Cancer cells also have other proteins that control their growth. In response to CDKs being blocked, they can rev up the production of these other proteins to compensate for the CDK inhibition. This can effectively render CDK inhibitors useless. One way to counteract this is to inhibit such compensatory pathways as well. Thus, Kisqali can be paired with endocrine (hormone) therapies, another class of drugs used to treat breast cancer.
Endocrine therapy (hormone therapy) blocks hormones, such as estrogen and progesterone. These hormones can interact with certain proteins — estrogen receptor (ER) and progesterone receptor (PR) — present on the surface of breast cancer cells and fuel their growth. Such cancers are termed hormone-receptor-positive (HR+) cancers. When these cancers are starved of hormones, they are not able to continue growing.
By pairing Kisqali and endocrine therapy, doctors can launch a multi-pronged attack that cannot be easily compensated for by breast cancer cells.
WATCH: Hormone Therapies for Breast Cancer: Aromatase Inhibitor
Letrozole is an aromatase inhibitor that blocks the aromatase enzyme, thereby preventing estrogen production. This helps slow down the growth of tumor cells sensitive to estrogen.
Zoladex (generic name: goserelin) is a type of endocrine (hormone) therapy.
Coping With Side Effects
Eggerts says her cancer treatment regimen has lingering side effects that are affecting her daily life. However, she remains optimistic and focused on the bigger picture.
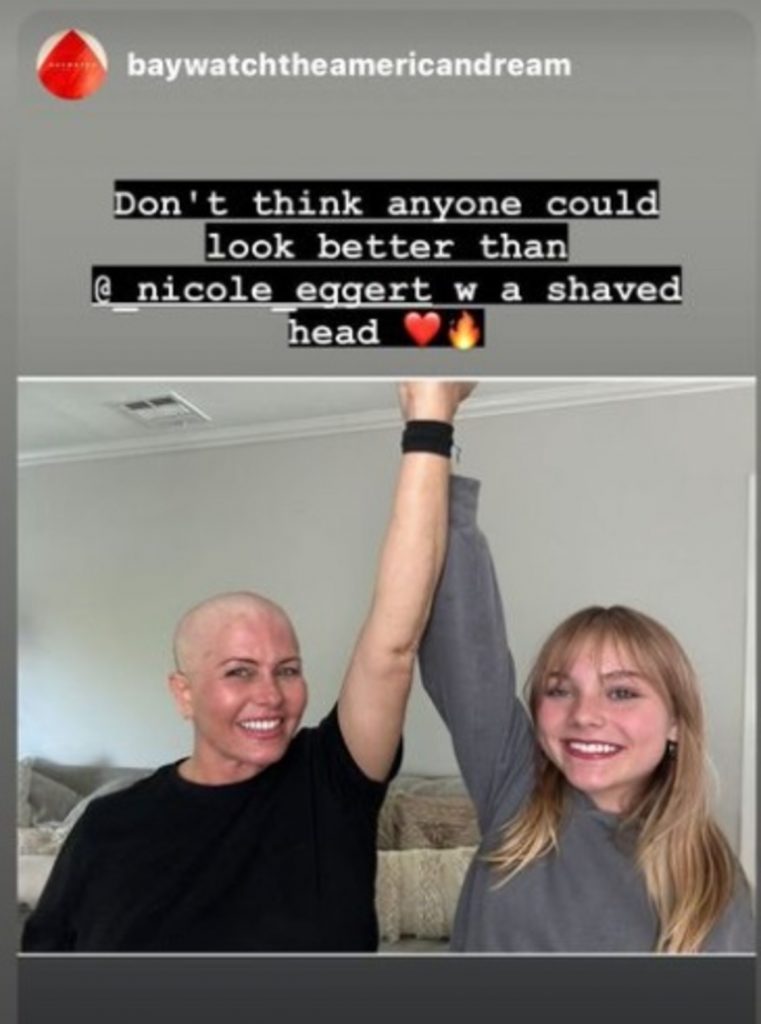
“My bones ache, my hair is falling out all over the place, hence why I’m shaving it tomorrow, my skin is dry, but these side effects are controllable, and I’m okay if it’s keeping the cancer away,” Eggert said.
During clinical trials, Kisqali was most commonly associated with nausea, vomiting, fatigue, diarrhea, and headaches. However, serious side effects can also occur. These include lung inflammation that may lead to trouble breathing or a cough. Severe skin reactions may also occur, including a rash, burning sensation, blisters, or skin peeling. Abnormal heart rhythms, liver problems, and a drop in blood cell counts have also been reported. Rarely, these serious side effects can lead to death.
Endocrine therapy can also bring about side effects such as hot flashes, night sweats, vaginal dryness, loss of sex drive, mood swings, joint pains, brittle bones when used long-term, and headaches.
Remaining Hopeful
Despite the rigors of treatment and the side effects, Eggert remains optimistic not just about her treatment but also about the future.
“I just want to live, I want to be here for my kids,” Eggert said.
View this post on Instagram
Eggert says resource outlets like SurvivorNet have helped her throughout her cancer journey, answering lingering questions that can arise on the spur of the moment.
“I read SurvivorNet all the time; it’s been a lifeline for me. As soon as I got my diagnosis, it popped up immediately in my feed, and SurvivorNet has really been one that I have really held onto.”
What To Ask Your Doctor
If you have been diagnosed with breast cancer, you may have questions about keeping your strength through treatment. Here are a few questions to help you begin the conversation with your doctor:
- What treatment will I be receiving?
- What side effects are associated with this treatment?
- Are there steps I can take daily to help minimize these side effects?
- What physical activity routine do you recommend for me during treatment?
- Do you have recommendations for someone who doesn’t particularly enjoy exercise?
- Can you recommend a dietitian who can help me with healthy eating tips and weight maintenance?
- I’ve been having trouble sleeping. Do you have any treatment recommendations?
Learn more about SurvivorNet's rigorous medical review process.

