Understanding NF1
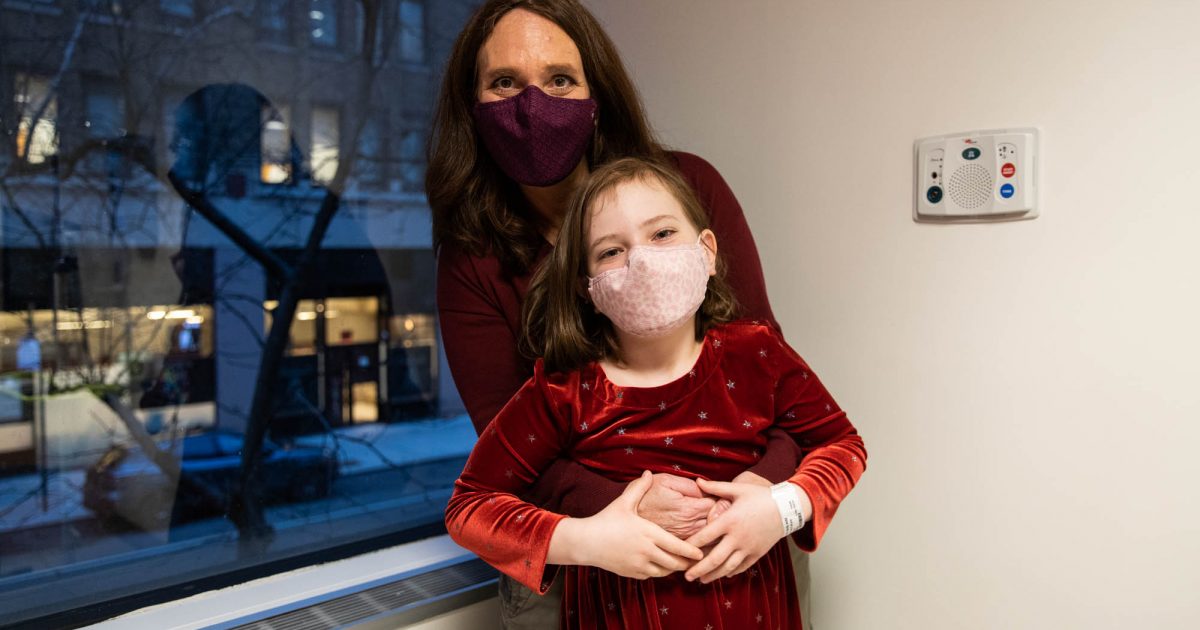
- Just in time for Christmas, NF1 patient Nora Osterman-Davis, 8, learned that her brain tumor is now 50% smaller, thanks to a clinical trial.
- NF1 is a rare genetic condition that causes benign tumors to grow on nerve tissue inside a person's brain and in the peripheral nervous tissue. Nora has a tumor growing inside her brain, obstructing her vision.
- Nora is part of a phase 3 clinical trial that has resulted in significant tumor shrinkage. Many SurvivorNet experts say that once they have exhausted all other treatment options for their patient, they will recommend looking into clinical trials.
The 8-year-old squealed with excitement as she pulled back the wrapping paper to reveal what was underneath: the Barbie Flippin Fun Gymnast playset.
Read More
"Getting a tumor to shrink is one thing that's good but also most importantly, for her the tumor had a functional consequence, meaning it had affected her vision," Dr. Nicolaides told SurvivorNet. "So, this has improved her vision significantly. That's the most important thing here."
Understanding NF1
Neurofibromatosis type 1, also known as NF1, is an incurable genetic condition that causes benign tumors to grow on nerve tissue inside a person's brain and in the peripheral nervous tissue. (Nora's mother, Heather Osterman-Davis, also has the condition, but it has not caused her any health problems. In fact, Heather explained that she had no idea she had the condition until she had children.)
However, Dr. Robyn Borsuk, a member of Nora's team and a clinical assistant professor in the Department of Pediatrics at Hassenfeld Children's Hospital, makes a good point: it is almost a misnomer to call Nora's tumor "benign." While the tumor growing inside Nora's brain is benign, meaning non-cancerous, its effect on the 8-year-old's life is not benign.
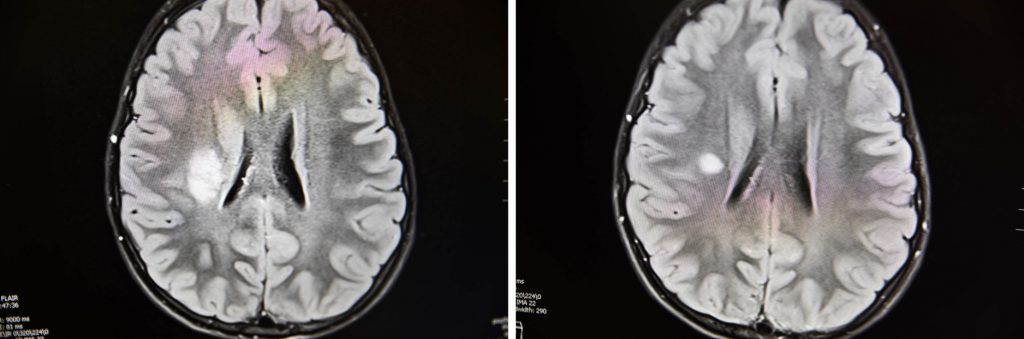
The tumor, which Nora and her family nicknamed "octapoop" (since it is shaped like an octopus), is obstructing Nora's vision.

NF1 is the most common type of neurofibromatosis, affecting about 1 in 3,000 people around the world, according to the Children's Tumor Foundation. Neurofibromatosis tumors are typically not cancerous, but sometimes, a benign tumor can become malignant. However, the good news is that most people with NF1 will never develop a malignant tumor.
The First Sign of Trouble
Over the summer, the Osterman-Davis family escaped their apartment in Manhattan's Greenwich Village and retreated to Pennsylvania for a lake-side vacation. That was when it all started.
"We went to the lake and I was on the dock I was reading a book with my grandma, and I was having trouble seeing some of the words," Nora explained. "That's when we started noticing (the tumor's symptoms.)"
The next day, Nora had a piano lesson. (Nora loves singing and music; she knows how to play quite a few songs on the piano, as well as one on the ukulele.)
"Some of the books have words to the song I play, and I couldn't see the words to the song I was playing," she said, adding that she tried to move the book closer to her eyes, then further away, but nothing seemed to allow the words to come into focus.
"I tried on my mom's glasses, and I still couldn't see (the words.) So then we went to the eye doctor. And you know how you look in the machine? None of the prescriptions worked. None of them," Nora said.
That is when Heather decided to reach out to Nora’s neurologist (NF1 specialist), who referred Nora to an ophthalmologist. The ophthalmologist set up an MRI scan, as well as pre-set Nora’s appointment with oncology, pending her MRI results. But that was when the worst was confirmed: Nora had a low-grade glioma on the optic pathway inside her brain.
Gliomas are not a specific type of brain tumor; glioma is a general term for tumors that start in glial cells. They are somewhat common as about three out of 10 of all brain tumors are considered gliomas, and most fast-growing brain tumors are categorized as gliomas. According to SurvivorNet expert Dr. Suriya Jeyapalan, director of medical neuro-oncology at Tufts Medical Center in Boston, there are about 22,000 new gliomas diagnosed in the United States each year.
Nora is among the 15% to 20% of children with NF1 who will develop a tumor in the optic pathway of their brain. According to research published in the U.S. National Library of Medicine, of that percentage, about 30% to 50% will be symptomatic from their glioma like Nora and about one-third of affected children will require therapeutic intervention again, like Nora. As you can see, she falls into a relatively rare category among her peers with NF1.
Nora explained that she cannot see anything small, or far away, but since the tumor has shrunk, she has gained some of her sight back.

The Clinical Trial & Nora's Progress
Nora's visit with Dr. Nicolaides serves the same purpose each month to check in and see how she is doing as a clinical trial participant. (Every three months, Nora's appointment is a bit longer as she has an MRI scan to check her tumor's shrinkage.)
She has just completed her fourth round of treatment; there are 24 treatment rounds in total. Twenty-four is kind of a lucky number for Nora, she told everyone in the room during her December appointment. "That's how many people I have in my class," she added.
Nora is part of a randomized phase 3 clinical trial for a MEK inhibitor called selumetinib (brand name: Koselugo). MEK inhibitors block proteins MEK1 and MEK2, which help control cell growth and survival, according to the National Cancer Institute.
Many SurvivorNet experts say that once they have exhausted all other treatment options for their patient, they will recommend looking into clinical trials. However, in some cases, such as Nora’s, the treatment being done in clinical trial can be more appealing than the standard of care. How can you find active clinical trials that may be right for you? Check out clinicaltrials.gov.
This website is a database that the U.S. government maintains. It compiles privately and publicly funded clinical trials conducted around the world. It can be a particularly useful resource for cancer patients with rare conditions as a tool for finding doctors who are experts on their diseases.

The trial randomly sorts participants into one of two treatment methods: the new treatment, selumetinib, or the "old fashioned way," as Dr. Nicolaides described it.
The "old fashioned" treatment method for NF1-related tumors requires weekly visits to a clinic where carboplatin and vincristine (chemotherapy) is administered via an intravenous port. (It should be noted that NF1 cannot actually be treated; Nora and other clinical trial patients are being treated for the tumors the condition causes.)
That chemotherapy treatment lasts about 64 weeks, while Nora's treatment with selumetinib requires her to take six pills per day three in the morning and three at night for 24 months. (She had never swallowed a pill prior to this clinical trial, so when she joined in August, she had to learn.) Patients being treated with intravenous chemotherapy often experience nausea and low blood counts, according to Dr. Nicolaides.
"(Nora's treatment method) is just much less brutal on the body," Heather said, adding that it also affords her daughter a better quality of life.
The U.S. Food and Drug Administration has already approved selumetinib as a treatment option for people with plexiform neurofibroma, which is a type of tumor that NF1 patients can get on their bodies, according to Dr. Nicolaides.
"But now the point is to see if this can be effective for brain tumors that patients with NF1 can get, or patients that don't have NF1 (who) can also get similar types of tumors that have a similar genetic susceptibility to these kinds of drugs," he added.
This is a national clinical trial, and Nora is the only patient at NYU Langone who is a current participant. Dr. Nicolaides explained that trial participants range in age, up to 21 years old.
"That's because there's a developmental window as children with NF1 are growing up, between the ages of 2 and 8 is when the bulk of them get these types of tumors; you're not going to have a 50-year-old with NF1 that gets this all of a sudden," he added.
Nora's Words of Wisdom
"Nora is the best hypewoman," one member of Nora's medical team said during her recent appointment.
"Nora is like living with the Hallmark Channel," Heather responded with a laugh.
As you can see, one of the things that keeps Nora going is her resilience and persistent positive attitude amid the trying situation she is faced with at just 8 years old.
She has some words of wisdom for other NF1 kids, or other children faced with dealing with a brain tumor:
"It can be a bit hard and stressful at first, but as you keep doing it, you can get used to it," Nora said. "And you can have a lot of people on your side that know what it's like (to have a brain tumor)."
But eventually, Nora added, "you'll be so used to it it'll just be like part of what you know how to do and then it's over!"
Learn more about SurvivorNet's rigorous medical review process.